-
Table of Contents
How to Identify the Right Insulin Type for You
Choosing the right type of insulin is a crucial decision for individuals managing diabetes. With various insulin types available, understanding their differences and how they align with your lifestyle and health needs is essential. This article will guide you through the process of identifying the right insulin type for you, supported by research, statistics, and real-life examples.
Understanding Insulin Types
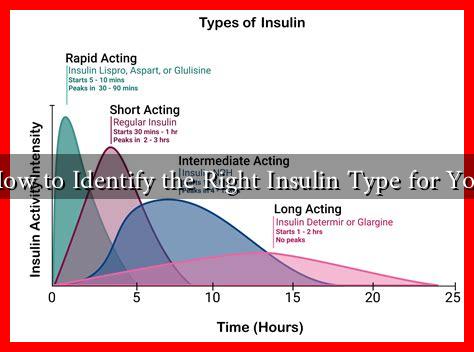
Insulin is a hormone that regulates blood sugar levels. For people with diabetes, insulin therapy is often necessary to maintain these levels within a healthy range. There are several types of insulin, categorized based on their onset, peak, and duration of action:
- Rapid-acting insulin: Begins to work within 15 minutes and lasts for 2-4 hours. Common examples include Lispro (Humalog) and Aspart (Novolog).
- Short-acting insulin: Takes about 30 minutes to start working and lasts for 3-6 hours. Regular insulin (Humulin R) is a typical example.
- Intermediate-acting insulin: Starts working in 2-4 hours and lasts for 10-16 hours. NPH (Humulin N) is a common type.
- Long-acting insulin: Takes several hours to start working and can last up to 24 hours or more. Examples include Glargine (Lantus) and Detemir (Levemir).
- Ultra-long-acting insulin: Provides coverage for more than 24 hours, such as Degludec (Tresiba).
Factors to Consider When Choosing Insulin
Identifying the right insulin type involves considering several factors:
- Type of diabetes: Type 1 diabetes typically requires insulin therapy from diagnosis, while Type 2 diabetes may be managed with lifestyle changes and oral medications initially.
- Blood sugar patterns: Monitoring your blood sugar levels can help determine how quickly and how long you need insulin to work.
- Daily routine: Your lifestyle, including meal times, exercise, and work schedule, can influence the type of insulin that best fits your needs.
- Personal preferences: Some individuals may prefer fewer injections or a specific delivery method, such as insulin pens or pumps.
Consulting Healthcare Professionals
Before making any decisions about insulin therapy, it is vital to consult with healthcare professionals. Endocrinologists, diabetes educators, and dietitians can provide personalized recommendations based on your medical history and lifestyle. They may conduct tests to assess your insulin sensitivity and overall health, which can inform the choice of insulin type.
For example, a case study published in the Journal of Diabetes Research highlighted a patient with Type 2 diabetes who switched from a long-acting insulin to a combination of rapid-acting and long-acting insulins. This change improved their blood sugar control significantly, demonstrating the importance of tailored insulin therapy.
Monitoring and Adjusting Insulin Therapy
Once you have started insulin therapy, continuous monitoring is essential. Regular blood sugar checks can help you and your healthcare team determine if your current insulin type and dosage are effective. Adjustments may be necessary based on:
- Changes in weight
- Alterations in diet or exercise
- Stress levels or illness
According to the American Diabetes Association, approximately 30% of people with Type 1 diabetes and 50% of those with Type 2 diabetes experience hypoglycemia (low blood sugar) at least once a year. Monitoring can help prevent such occurrences and ensure optimal insulin management.
Conclusion
Identifying the right insulin type for you is a multifaceted process that requires careful consideration of your diabetes type, lifestyle, and health needs. By understanding the different types of insulin, consulting healthcare professionals, and continuously monitoring your blood sugar levels, you can make informed decisions that lead to better diabetes management. Remember, the goal is to find an insulin regimen that fits seamlessly into your life while effectively controlling your blood sugar levels. Always stay informed and proactive in your diabetes care journey.